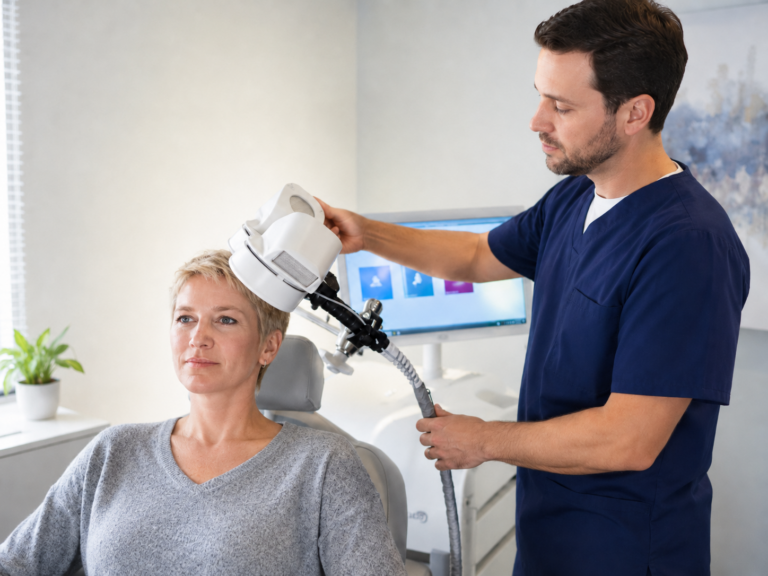
Can TMS Help With Brain Fog? What to Expect Before, During, and After

Caleb Whitenack, MD

If you have been living with brain fog, you already know how disruptive it can be. It is not just the forgetfulness or the mental slowness. It is the feeling that your mind used to work differently, that thinking clearly once came naturally, and that somewhere along the way it stopped. Simple things that never required effort now do. That gap is exhausting in a way that is difficult to explain to people who have not experienced it.
Before diving into what TMS can offer, it helps to understand one important clarification: brain fog is a symptom, not a standalone diagnosis. This means TMS does not target brain fog directly. What it does is address the underlying conditions that cause it, and for many patients, improved mental clarity follows as part of that process.
What Is Brain Fog?
You may have noticed that no doctor has ever written “brain fog” on a diagnosis form. That is because it is not a medical condition on its own. Clinically speaking, brain fog refers to a cluster of cognitive symptoms that can include:
- Difficulty concentrating or staying focused
- Memory lapses and forgetfulness
- Slowed thinking and processing
- Persistent mental fatigue that rest does not fully relieve
There is always something driving the brain fog. Depression, anxiety, chronic illness, hormonal changes, and long COVID are among the most common underlying causes. Getting to the root of what is behind your brain fog is what makes treatment meaningful, and it is where TMS becomes relevant.

Why TMS May Help With Brain Fog
To understand why TMS may help, it is worth knowing briefly how it works. Transcranial magnetic stimulation (TMS) delivers focused magnetic pulses to specific regions of the brain, most commonly the prefrontal cortex, which is the area responsible for attention, decision-making, and emotional regulation. These pulses stimulate neural activity and encourage the brain to form and strengthen new connections, a process known as neuroplasticity and how the brain learns to heal.
TMS also influences how the brain produces and regulates neurotransmitters, including serotonin and dopamine, both of which play a meaningful role in cognitive function. A recently published systematic review found that high-frequency rTMS applied to the prefrontal cortex produced measurable improvements in cognitive accuracy and executive function, suggesting the cognitive effects of TMS extend beyond mood regulation into areas directly relevant to brain fog. The clinical evidence base in this area continues to grow.
Conditions Where TMS May Ease Brain Fog
If you are exploring TMS for brain fog, the most important question is not whether TMS helps with brain fog in general. It is whether TMS treats the specific condition that is causing your brain fog. Here is where the evidence currently stands.
Depression
If your brain fog is rooted in depression, it helps to understand how TMS therapy for depression works and why the clinical case for it is among the strongest. Depression does not only affect mood. It also disrupts cognitive function in ways that can feel just as debilitating, including slowed processing speed, difficulty retaining information, and a mental heaviness that makes even routine thinking feel labored. TMS is FDA-cleared for major depressive disorder, and a real-world study found significant improvement in both depressive and cognitive symptoms in patients treated with rTMS, suggesting the cognitive benefits are a meaningful part of the treatment outcome rather than a secondary effect.
Anxiety
If chronic anxiety is part of your picture, it may be contributing to your brain fog more than you realize. Sustained anxiety keeps the nervous system in a prolonged state of activation, which over time quietly erodes concentration and working memory. TMS targets prefrontal regions involved in both emotional and cognitive regulation, and for many patients, as anxiety symptoms begin to ease through treatment, the mental cloudiness that accompanies them tends to lift as well.
Long COVID
If your brain fog developed or worsened following a COVID-19 infection, you are not imagining it and you are not alone. Persistent cognitive difficulties following infection have become a significant area of clinical research. Contributing factors being studied include neuroinflammation, disrupted cerebral blood flow, and the psychological toll of prolonged illness. A 2023 study published in Progress in Rehabilitation Medicine was among the first to examine rTMS specifically for long COVID cognitive dysfunction, with participants showing measurable improvements in both fatigue and cognitive performance. This remains an investigational application, and a qualified provider can help determine whether it may be appropriate in your situation.
ADHD
If attention and executive function challenges are at the center of your brain fog experience, including difficulty sustaining focus, organizing tasks, and filtering out distractions, ADHD may be a contributing factor worth exploring. TMS use for ADHD is currently off-label, meaning it falls outside its FDA-cleared indications, but emerging research suggests it may support attentional regulation by stimulating prefrontal activity.
Chronic Fatigue Syndrome and Fibromyalgia
If you are living with chronic fatigue syndrome or fibromyalgia, you are likely familiar with the cognitive burden these conditions carry. Patients commonly report:
- Persistent mental fatigue that does not resolve with rest
- Difficulty concentrating on routine tasks
- Slowed information processing throughout the day
TMS is being explored as a complementary option for patients whose cognitive symptoms persist despite other treatments, though the evidence base in this area is still developing.
What to Expect From TMS Treatment
One of the most valuable things you can do before starting TMS is understand what the experience actually looks like from beginning to end. The path through treatment is not always linear, and knowing what is normal at each phase can help you stay steady when things feel uncertain.
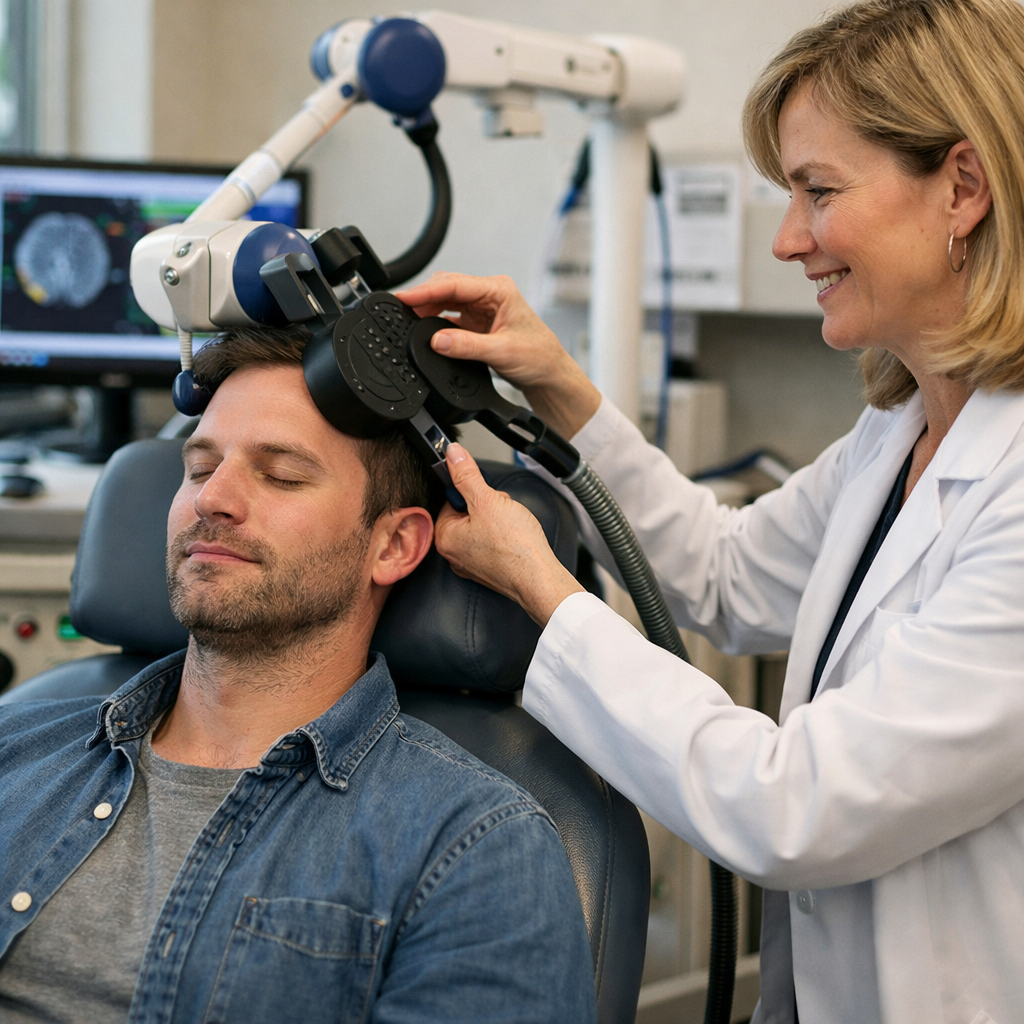
Before Treatment
Your journey starts with a thorough clinical evaluation. A qualified TMS provider will review your symptoms, medical history, and any previous treatments to determine whether TMS is appropriate for your situation and which underlying condition may be driving your cognitive symptoms. TMS is not a one-size-fits-all protocol, and the more precisely your provider understands your presentation, the more effectively treatment can be tailored to you.
During Treatment
A standard TMS course typically looks like this:
- Daily sessions five days a week over six to eight weeks
- Each session lasting approximately 30 minutes
- No sedation, no anesthesia, and no recovery time required
- You can return to your normal activities immediately after each session
Cleveland Clinic notes that most patients experience mild or no side effects throughout treatment. This is consistent with findings from a pivotal TMS safety trial, where the NIMH reported that fewer than 5.5% of patients discontinued due to side effects and no adverse effects on cognition were observed.
That said, some patients do experience a temporary increase in fatigue or mental heaviness during the early sessions, sometimes called a treatment dip. This is a recognized pattern rather than a sign that treatment is not working. If that happens to you, staying in close contact with your provider matters. They can monitor your response, make adjustments if needed, and help you distinguish between a normal early-phase experience and something that deserves closer attention.
After Treatment
For many patients, cognitive clarity tends to build gradually and cumulatively rather than arriving all at once. Many people describe it as subtle at first, finding it a little easier to follow a conversation, hold onto a thought, or move through tasks that previously felt out of reach, before noticing broader improvements in the weeks that follow. A follow-up appointment after completing your course gives your provider the opportunity to evaluate your response and discuss whether any maintenance sessions may be appropriate.
Final Thoughts
TMS is most likely to be a meaningful option when your brain fog is connected to a condition it is known to treat, particularly depression or anxiety. If your cognitive symptoms seem more closely tied to lifestyle factors such as disrupted sleep, nutritional gaps, or chronic stress, those areas are generally worth addressing first.
The right starting point is a conversation with a qualified psychiatric provider. They can review your history, help clarify what may be driving your symptoms, and determine together with you whether TMS is an appropriate next step in your treatment plan.
Frequently Asked Questions (FAQs)
1. How many TMS sessions does it take to see results for brain fog?
Most standard TMS protocols involve 20 to 36 sessions delivered over four to eight weeks. Some patients begin noticing cognitive changes within the first few weeks, while others experience more significant improvements toward the end of or following the full course.
2. Is TMS covered by insurance for brain fog?
Insurance coverage for TMS is typically tied to its FDA-cleared indications, most commonly treatment-resistant depression. If TMS is being recommended as part of treatment for a covered diagnosis, your plan may cover it, so verifying benefits with your provider before beginning is always advisable.
3. Can TMS make brain fog worse before it gets better?
Some patients do experience a temporary increase in fatigue or mental heaviness in the early sessions, commonly referred to as a treatment dip. This is not universal, but it is a recognized pattern and generally resolves as treatment continues.
4. How is TMS different from medication for brain fog?
Unlike medication, TMS does not introduce any substance into the body and carries no systemic side effects such as weight changes, sleep disruption, or dependency risk. It works by directly stimulating targeted brain regions, making it a distinct option for those who have not responded adequately to pharmacological approaches.
Responsibly edited by AI
Other Blog Posts in
Animo Sano Psychiatry is now serving patients across multiple states. If you’d like to schedule an appointment, please contact us to get started.
Get Access to Behavioral Health Care
Let’s take your first step towards. Press the button to get started. We’ll be back to you as soon as possible.ecovery, together.