You’ve done the therapy. You’ve tried the medication. Maybe you’ve tried more than one of each. And you’re still not okay. If that’s where you are, you’re not out of options — and you’re not alone. Transcranial Magnetic Stimulation (TMS) is a non-invasive brain stimulation treatment that’s increasingly being used for people living with PTSD, especially when standard treatments haven’t brought enough relief. This post explains what the research actually shows, which symptoms TMS may help with, and what you can realistically expect — including the things most people aren’t told before they start.
Why Standard Treatments Don’t Always Work for PTSD
Therapy and medication are the frontline treatments for PTSD — and for many people, they help significantly. But a meaningful number of people go through multiple rounds of trauma-focused therapy, try several medications, and still find themselves stuck. That’s not a failure of effort. It reflects how complex and deeply rooted trauma can be in the brain.
This is where TMS enters the conversation. TMS (Transcranial Magnetic Stimulation) is a non-invasive procedure that uses magnetic pulses to stimulate specific areas of the brain involved in mood regulation and fear processing. It’s used off-label for PTSD — meaning it’s applied based on growing clinical evidence rather than a formal FDA indication — and it’s an option being offered for the right candidates when other treatments haven’t been enough.
The APA’s 2024 position statement on TMS acknowledges that access to TMS for evidence-based indications beyond depression remains an important clinical priority — reflecting the growing body of research supporting its use across conditions. For many people living with treatment-resistant PTSD, TMS represents a genuinely different kind of option: one that works on the brain directly, without medication, and without requiring you to re-expose yourself to trauma in the way some therapies do.

PTSD and Depression Often Co-Occur — and That Matters for TMS
PTSD rarely travels alone. Research shows that between 30% and 50% of people living with PTSD also meet criteria for major depression — and that overlap is clinically important when it comes to TMS.
A large VA study found that among patients who received a full course of TMS for depression, nearly 46% of those who also had PTSD no longer met diagnostic criteria for PTSD after treatment. That’s a meaningful finding — not because TMS was targeting PTSD directly in those cases, but because the brain regions involved in depression and trauma response are closely connected.
TMS works by delivering magnetic pulses to the prefrontal cortex, the part of the brain responsible for emotional regulation, decision-making, and moderating fear responses. In people with PTSD, this region tends to be underactive — which helps explain why the brain’s alarm system stays on high alert even when there’s no real threat. By stimulating that area, TMS may help restore some of that regulatory capacity.
This also means that for many people, the emotional weight of PTSD and depression feeding into each other isn’t just one condition — it’s two reinforcing each other, and TMS may be able to address both at once.
Which PTSD Symptoms May Respond to TMS?
This is one of the most common questions people ask before starting TMS, and the honest answer is: it varies. But here’s what the research and patient experience suggest may improve:
- Intrusive memories and flashbacks — the involuntary re-experiencing of traumatic events
- Hypervigilance — the constant state of alertness that makes it hard to feel safe anywhere
- Nightmares — particularly those tied to re-experiencing trauma during sleep
- Emotional numbing — the disconnection from feelings, people, and things you used to care about
- Irritability and emotional reactivity — the hair-trigger responses that strain relationships
- Concentration and memory difficulties — the cognitive fog that often accompanies PTSD
- Sleep disruption — PTSD and sleep have a particularly difficult relationship that goes beyond just having bad nights
It’s important to frame this accurately: TMS rarely eliminates PTSD entirely. Most people experience partial improvement — enough to meaningfully shift quality of life, but not necessarily a complete resolution. Clinical research on TMS for PTSD has shown response rates that are promising, particularly for those who haven’t responded to first-line treatments.
Can TMS Make PTSD Symptoms Temporarily Worse?
This is something people ask in forums and support communities all the time — and it deserves a direct answer: yes, for some people, emotional intensity can increase in the early weeks of TMS treatment.
This isn’t a sign that the treatment is failing. It’s actually a known phenomenon, and your provider should tell you about it before you start.
Here’s one way to understand it: TMS begins to activate brain regions that trauma may have quieted over time. As those regions “wake up,” some people find that emotions — including difficult ones — become more accessible. What felt numb may start to feel raw before it starts to feel better. This process, when it happens, typically settles as treatment continues.
If you’re experiencing this, the most important thing is to tell your provider. Don’t stop treatment on your own without talking to them first. Adjustments can be made — and in many cases, what feels like a step backward is actually the beginning of the brain starting to reorganize.
Who Might Be a Good Candidate for TMS for PTSD?
TMS for PTSD tends to be most appropriate for people who:
- Have tried trauma-focused therapy (such as CPT, EMDR, or prolonged exposure) with limited results
- Have tried medication without adequate relief, or cannot tolerate medication side effects
- Are living with both PTSD and depression, where there’s meaningful overlap to address
- Are medically cleared for TMS (there are some contraindications, such as a history of seizures or certain metal implants near the head)
TMS is not a replacement for therapy — and for most people, it works best alongside it. Someone who has built some stability through trauma-focused care may actually respond better to TMS than someone starting from scratch, because the brain has already begun doing some of the work. And for those considering TMS specifically, the evaluation process helps determine whether the timing and fit are right before any treatment begins.
Candidacy is always determined through a clinical evaluation with your TMS provider. If you’re wondering whether TMS might be appropriate for you, the best first step is a conversation.
What to Expect During TMS Treatment for PTSD

TMS is done as an outpatient procedure — no anesthesia, no sedation, no hospital stay. You come in, have your session, and go about your day.
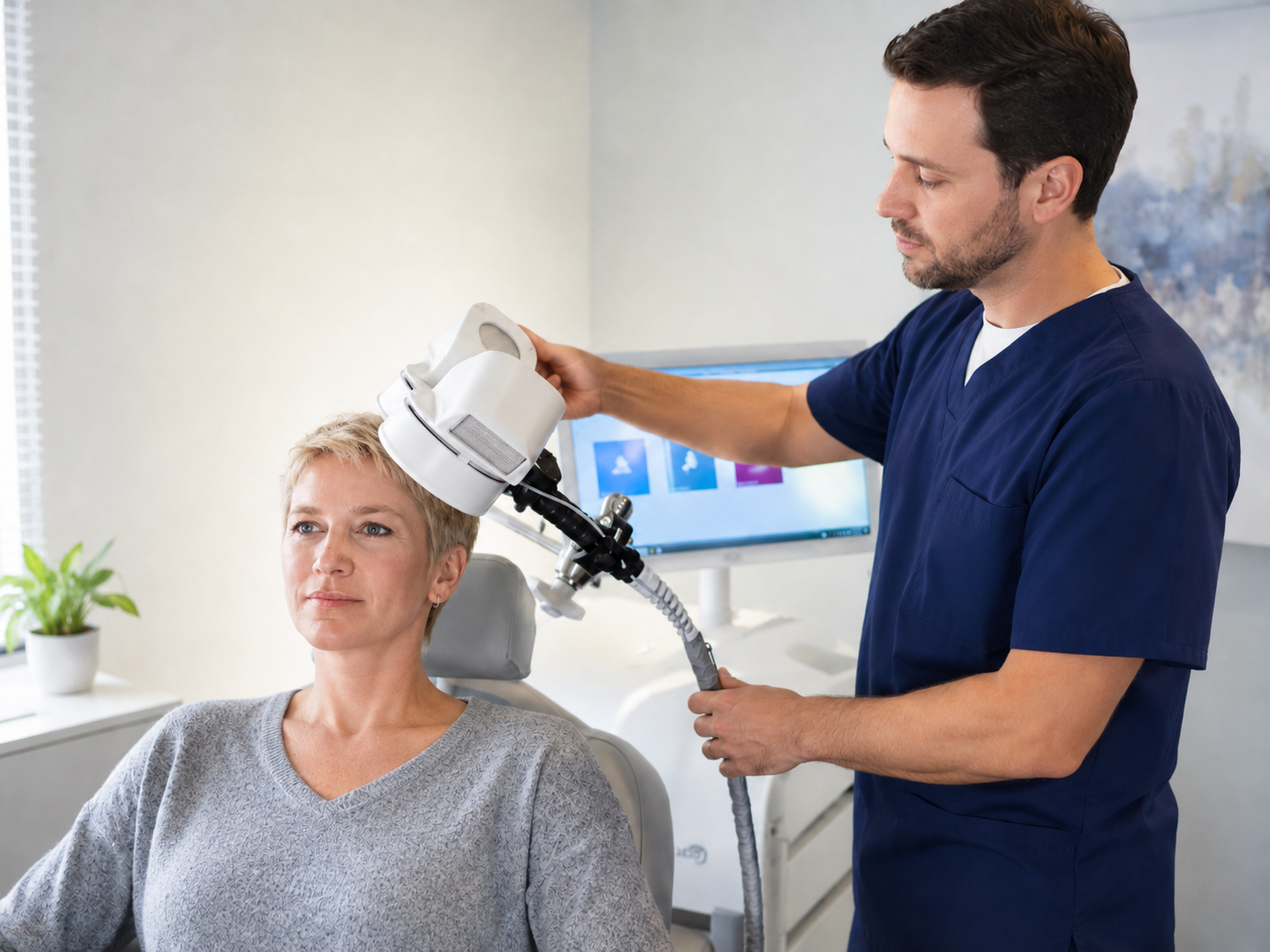
A typical TMS course involves daily sessions five days a week over roughly seven weeks. Each session lasts between 20 and 40 minutes. You’ll sit in a chair while a magnetic coil is placed against your scalp. Most people describe the sensation as a repetitive tapping or light knocking feeling. It can be mildly uncomfortable at first, but the majority of patients adjust within the first few sessions.
Don’t expect dramatic results in the first week or two. TMS works gradually and cumulatively. Most people begin noticing changes somewhere between weeks two and four — sometimes sooner and sometimes later. If you reach week four without feeling any shift, that’s a signal to talk to your provider, not a reason to assume it’s not working.
Progress is rarely linear. There may be days mid-treatment that feel harder than the days before you started. That doesn’t mean treatment is failing — but it does mean that having a provider you can communicate with openly is essential.
Final Thoughts
PTSD is one of the most difficult things a person can live with — not just because of what happened, but because of how it changes the brain, the body, and the sense of what’s possible. If you’ve done the work and still don’t feel like yourself, that’s not a personal failure. It means you may need a different kind of support.
TMS won’t be the right answer for everyone. But for the right person, at the right time, with the right clinical team behind them, it can open a door that felt permanently closed. That’s worth knowing about. And it’s worth asking your provider about.
Frequently Asked Questions (FAQs)
1. Is TMS covered by insurance for PTSD?
It depends on your plan. Because TMS for PTSD is off-label, coverage is inconsistent. Some insurers will cover it — especially when depression is also present — while others won’t. Call your insurance provider before starting treatment to confirm.
2. Can TMS be used alongside therapy for PTSD?
Yes, and it often works better that way. TMS and trauma-focused therapy like EMDR or CPT address different things, and combining them may improve outcomes for some people.
3. How is TMS for PTSD different from TMS for depression?
The protocol is often similar — both target the prefrontal cortex. The difference is in what’s being tracked. For PTSD, providers monitor trauma-specific symptoms like flashbacks and hypervigilance, not just mood.
4. How long does it take to see results from TMS for PTSD?
Most people begin noticing changes between weeks two and four. Some don’t see improvement until the full course is complete. Results are gradual — a full course typically runs four to six weeks.
5. What if TMS doesn’t work for my PTSD?
Not everyone responds, and that’s worth acknowledging honestly. If TMS doesn’t help, there are still other options to explore with your provider. Not responding to one treatment doesn’t mean you’ve run out of paths forward.
Responsibly edited by AI
Other Blog Posts in
Animo Sano Psychiatry is now serving patients across multiple states. If you’d like to schedule an appointment, please contact us to get started.
Get Access to Behavioral Health Care
Let’s take your first step towards. Press the button to get started. We’ll be back to you as soon as possible.ecovery, together.






