Understanding Depression Relapse Without Shame

Stefanie Solomon, PA-C, CAQ-PSY

Depression relapse after a period of recovery is one of the most disorienting experiences a person can face. There’s often a quiet devastation that comes with it — not just the symptoms themselves, but the thought: I was doing so well. What went wrong?
The answer, in most cases, is nothing went wrong. Depression is a highly recurrent condition, and returning to it does not reflect personal failure. It reflects biology. Understanding why relapse happens, what makes a second episode different from the first, and how to approach it differently can change the entire trajectory of care.
How Common Is Depression Relapse?
The statistics on depression recurrence are striking — and worth knowing, because they reframe relapse as a medical event rather than a personal one.
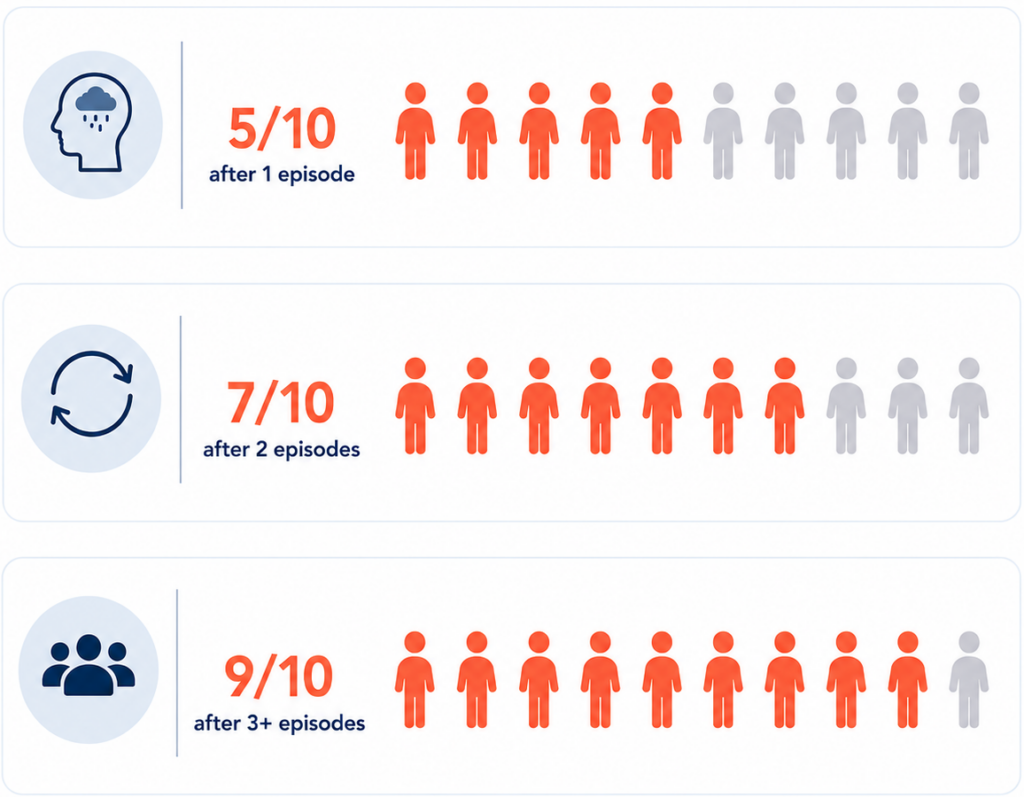
At least 50% of people who recover from a first depressive episode will go on to have a second one. After two episodes, the risk rises to 70%, and after three or more, it reaches approximately 90%. A prospective 10-year study published in the American Journal of Psychiatry found that nearly two-thirds of subjects suffered at least one recurrence, and that the risk increased by 16% with each successive episode.
These numbers are not meant to discourage — they are meant to contextualize. Depression recurrence is the norm, not the exception. It is a pattern the medical community has studied and documented extensively, and it is one that can be planned for.
Relapse vs. Recurrence: What Is the Difference?
These two terms are often used interchangeably, but they describe distinct experiences.
A relapse refers to the re-emergence of depressive symptoms during the recovery phase — before full remission has occurred. A recurrence is a new depressive episode that begins after a person has fully recovered. Research indicates that the majority of relapses — around 79% — occur within the first six months following treatment, which is why the period immediately after improvement is clinically significant.
Depression doesn’t always look the same the second time around, either. Symptoms may be subtler, more physical, or show up differently than before — which is one reason why understanding signs of depression relapse can help patients and families recognize what a returning episode actually looks like in practice.
Why Stopping Medication Too Soon Triggers Recurrence?
One of the most common — and most preventable — drivers of depression relapse is discontinuing antidepressant medication when symptoms improve. Feeling better is not the same as being recovered. The brain needs time to consolidate that improvement at a neurological level.
Antidepressants work by stabilizing neurotransmitter activity over time. Stopping them prematurely — particularly without clinical guidance — removes a protective layer the brain may still depend on. Residual symptoms that remain after partial recovery are one of the strongest clinical predictors of a full episode returning.
Evidence indicates that for patients still at appreciable risk after 4 to 6 months of treatment, continuing antidepressant medication may halve the risk of relapse for up to two years. This is why medication management in depression isn’t just about finding the right prescription — it’s also about having ongoing clinical guidance around when and how to safely adjust or discontinue it.
What a Second Episode Teaches?
A second depressive episode is painful. It is also informative. It often reveals patterns — specific triggers, early warning signs, which treatments worked and which didn’t — that weren’t visible during the first episode.
Depression symptoms may shift in the second episode, timing may differ, and what helped before may need adjustment. This is not a sign that treatment is failing — it is a signal that care needs to be personalized more precisely.
A second episode also creates an opportunity to address what may have been missed initially. Comorbid anxiety, unresolved trauma, sleep disruption, or incomplete remission from the first episode are all factors that increase recurrence risk and deserve direct attention. Sometimes depression occurs in a way which is unrecognizable. Melancholic depression is one of those, it manifests through “somatic” or physical symptoms rather than being a reaction to external stress.
Episodic Depression vs. Chronic Depression
Not all depression follows the same pattern, and understanding the distinction matters for long-term planning.
Episodic depression involves discrete episodes with periods of full recovery between them. Chronic depression — sometimes called persistent depressive disorder — involves symptoms that persist for two years or longer without full remission. The treatment approach, medication strategy, and long-term goals differ significantly between these two presentations.
This is why an accurate psychiatric diagnosis matters at every stage, including after a recurrence. A thorough evaluation can determine whether the current episode represents a new acute event or evidence of a more persistent pattern that requires a different clinical approach.
Having a Relapse Plan Before It Is Needed
One of the most protective things a person can do is develop a relapse plan during a period of wellness — not in the middle of a crisis.
A practical relapse plan includes knowing which provider to contact and how to reach them quickly, understanding what changes in sleep, appetite, or social withdrawal mean in context, and identifying one or two trusted people who can provide honest feedback about behavioral changes.
Mindfulness-based cognitive therapy (MBCT) has strong clinical evidence for reducing depression relapse risk, particularly for those who have experienced three or more episodes. It teaches pattern recognition and early response skills that extend well beyond the treatment period itself. Structured therapy — whether CBT, MBCT, or another evidence-based modality — is a core part of psychotherapy and an important complement to medication management in preventing recurrence.
Why Returning to Care Earlier Always Produces Better Outcomes?

A persistent barrier to seeking help after a relapse is shame — the sense that returning to treatment represents a regression. It does not. The severity of depression and resistance to treatment increases with each successive episode, which means early intervention at the first sign of returning symptoms carries genuine clinical weight.
Returning to a provider at the first signs of recurrence — rather than waiting until symptoms are severe — shortens episode duration, prevents escalation, and preserves the neurological gains made during prior treatment. Reaching out early is a clinical decision, not a concession.
Depression that goes unaddressed long enough can also intersect with broader mental health challenges that make recovery more complex. If returning symptoms feel familiar, reaching out sooner rather than later is always the right call.
Final Thoughts
Depression returning is not evidence that something is broken. It is evidence that depression is a medical condition with a known recurrence pattern — and one that responds well to timely, personalized treatment. The second episode, while difficult, often comes with more self-awareness, more clinical information, and more tools than the first. With the right care and a proactive plan, relapse does not have to define the trajectory. It can redirect it.
Frequently Asked Questions (FAQs)
1. Is depression relapse a sign that treatment didn’t work?
Not necessarily. Depression is a highly recurrent condition regardless of treatment quality. Relapse is common even after successful treatment and does not mean the previous approach failed.
2. How soon can depression return after recovery?
It depends on whether symptoms return during recovery or after it. Research indicates that the majority of relapses — where symptoms re-emerge before full remission is reached — occur within the first six months of treatment. A true recurrence, meaning a new depressive episode after full recovery, tends to follow a longer timeline. The average gap between a first and second episode is approximately 4.5 years. Both possibilities make ongoing clinical follow-up important — especially in that first post-treatment year.
3. Can depression be prevented from returning?
Recurrence can be significantly reduced — though not always prevented — through continued treatment, therapy, lifestyle factors, and regular psychiatric follow-up. A relapse prevention plan developed with a provider is one of the most effective tools available.
4. When should professional support be sought after a relapse?
As early as possible. At the first signs of returning to low mood, sleep changes, or withdrawal from daily life, contacting a psychiatric provider is the right step — not a last resort.
Responsibly edited by AI
Other Blog Posts in
Animo Sano Psychiatry is now serving patients across multiple states. If you’d like to schedule an appointment, please contact us to get started.
Get Access to Behavioral Health Care
Let’s take your first step towards. Press the button to get started. We’ll be back to you as soon as possible.ecovery, together.





