Depression After Retirement: Why It Happens and What Helps

Jasmine Zaman – PA-C

Retirement is supposed to feel like freedom. No more deadlines, early mornings, or workplace stress. But for many retirees, the weeks and months that follow feel unexpectedly flat — sometimes even hollow. What was supposed to be a reward can quietly become one of the most psychologically challenging transitions of a person’s life.
That’s because retirement isn’t just a lifestyle change — it’s an identity shift. For decades, work shapes how people spend their time, how they see themselves, and how they connect with others. When that structure disappears almost overnight, the emotional fallout can be significant. Feelings of purposelessness, loneliness, and low mood can settle in gradually — and because they don’t look the way most people expect depression to look, they often go unrecognized for months. Understanding why this happens is the first step toward doing something about it.
How Common Is Retirement Depression?
The numbers are striking. A peer-reviewed meta-analysis found the prevalence of depression in retirees to be approximately 28% — nearly one in three people. One frequently cited study found that self-reported depression increases by 40% during the first few retirement years. And yet most retirement planning conversations focus almost entirely on finances, not on the psychological weight of leaving a career behind.

Why Does Depression After Retirement Occur?
The emotional impact of retirement is rarely caused by a single factor. Instead, it tends to develop from a combination of subtle yet meaningful life changes.
1. Loss of Identity and Purpose
For decades, work provides more than income. It shapes identity, daily structure, and a sense of contribution. When that role ends, individuals may find themselves asking a difficult question: What now?
Without a clear answer, feelings of emptiness or lack of direction can begin to surface.
2. Sudden Loss of Routine
Workdays create a predictable rhythm—waking up at a set time, engaging in tasks, interacting with others. Retirement removes that structure almost overnight.
Abrupt shifts can lead to emotional instability, particularly when no new routine replaces the old one.
3. Social Disconnection
Work environments often provide regular social interaction. After retirement, those daily connections may decrease significantly.
Over time, reduced social engagement can contribute to loneliness, which is closely linked to depressive symptoms in older adults.
4. Financial Stress and Uncertainty
Even when retirement is planned, financial concerns can remain. Questions about long-term savings, healthcare costs, or supporting family members can create ongoing stress.
This underlying anxiety can gradually contribute to depressive symptoms.
5. Health Changes and Aging
Physical health challenges often become more noticeable in later life. Chronic illness, reduced mobility, or fatigue can limit daily activities and independence.
These changes can reinforce feelings of loss, further impacting emotional well-being.
Recognizing Symptoms of Depression in Retirement
Depression after retirement does not always appear as obvious sadness. In many cases, it presents more subtly.
Common symptoms may include:
- Persistent low mood or emotional numbness
- Loss of interest in previously enjoyable activities
- Fatigue or low energy
- Changes in sleep patterns (sleeping too much or too little)
- Difficulty concentrating or making decisions
- Changes in appetite or weight
- Feelings of worthlessness or guilt
These symptoms can develop gradually, making them easy to overlook or dismiss as a “normal” part of aging. However, they are not inevitable—and they are treatable.
When Retirement Improves Mental Health
It is equally important to recognize that retirement does not always lead to depression. For some individuals, stepping away from workplace stress can significantly improve mental health.
In fact, certain studies indicate a reduction in depression risk in the years following retirement, particularly when individuals maintain an active and engaged lifestyle .
This suggests that the impact of retirement depends largely on how the transition is managed.
Coping Strategies for Retirement Depression
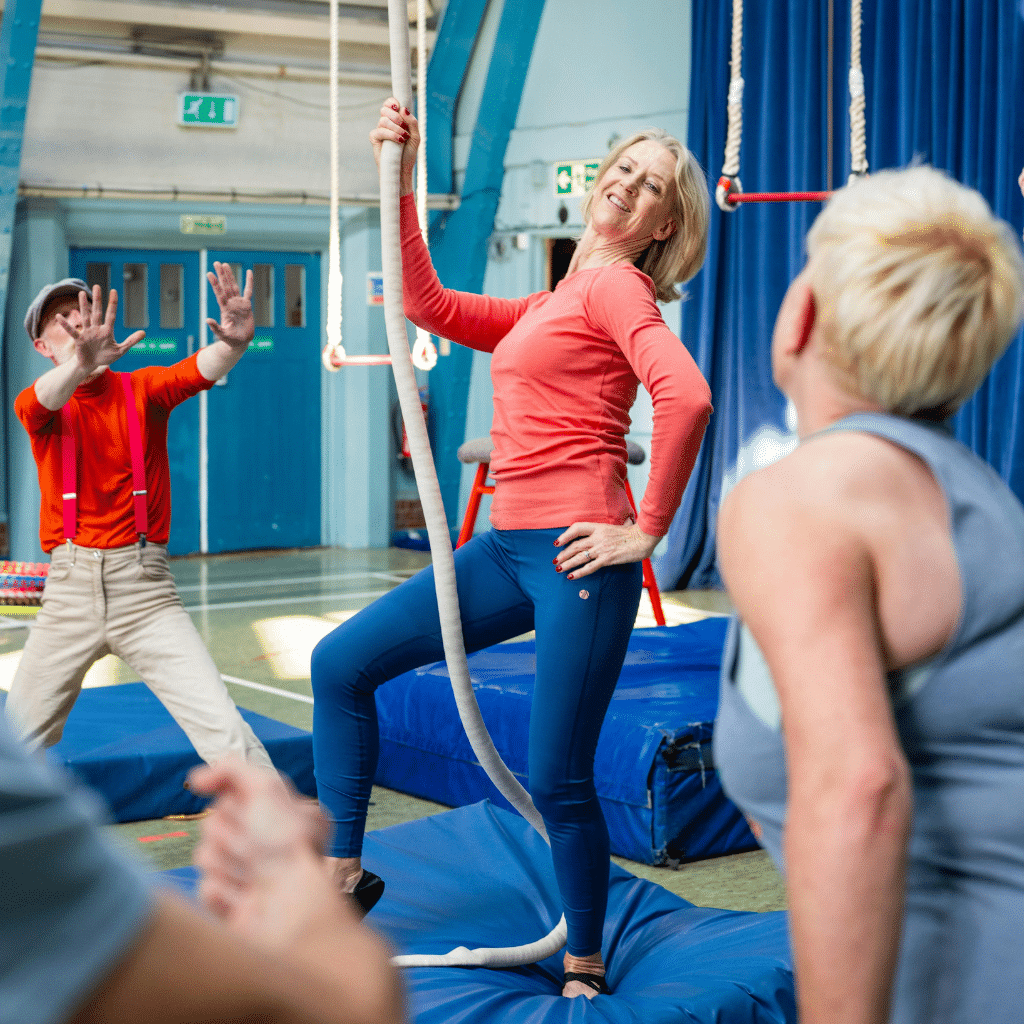
- Build a new routine. The loss of daily structure is one of the most underestimated parts of retirement. A new schedule — even a loose one — gives the nervous system something to anchor to.
- Stay socially connected. This requires more intentional effort after retirement. Volunteering, community groups, or simply scheduling regular time with people who matter aren’t optional — they’re protective.
- Find new sources of purpose. Purpose doesn’t retire when a career ends. Mentoring, learning new skills, part-time work, or creative pursuits can restore the sense of contribution that work once provided. The American Psychological Association has resources on healthy aging and purpose worth exploring.
- Support physical health. Exercise, sleep, and nutrition have a direct and measurable impact on mood. Physical decline that goes unmanaged deepens depressive symptoms over time.
- Seek professional support when needed. When symptoms have been present for two weeks or more and are interfering with daily life, that’s worth taking seriously — not waiting out. Cognitive Behavioral Therapy (CBT) and psychiatric medication management are both effective, evidence-based options.
Final Thoughts
Retirement is one of the largest identity and lifestyle transitions most people will ever face — and the emotional side of it deserves just as much planning as the financial side. Depression after retirement is common, often goes unrecognized, and is frequently dismissed as a normal part of aging. It isn’t. With the right support, this chapter of life can hold genuine meaning, connection, and purpose. It sometimes just takes a little help getting there.
Frequently Asked Questions (FAQs)
1. Is depression after retirement normal?
It’s common, but not inevitable. Nearly one in three retirees experience depressive symptoms. It is not a character flaw, and it responds well to treatment.
2. How long does it last?
It varies. Without support, it can persist for months or years. Early intervention typically leads to better outcomes.
3. When should someone seek professional help?
When low mood, loss of interest, fatigue, or withdrawal have been present for two or more weeks and are affecting daily functioning, a clinical evaluation is the right next step.
Responsibly edited by AI
Other Blog Posts in
Animo Sano Psychiatry is now serving patients across multiple states. If you’d like to schedule an appointment, please contact us to get started.
Get Access to Behavioral Health Care
Let’s take your first step towards. Press the button to get started. We’ll be back to you as soon as possible.ecovery, together.





