Combining Medication With TMS Therapy: A Holistic Treatment Roadmap

Caleb Whitenack, MD
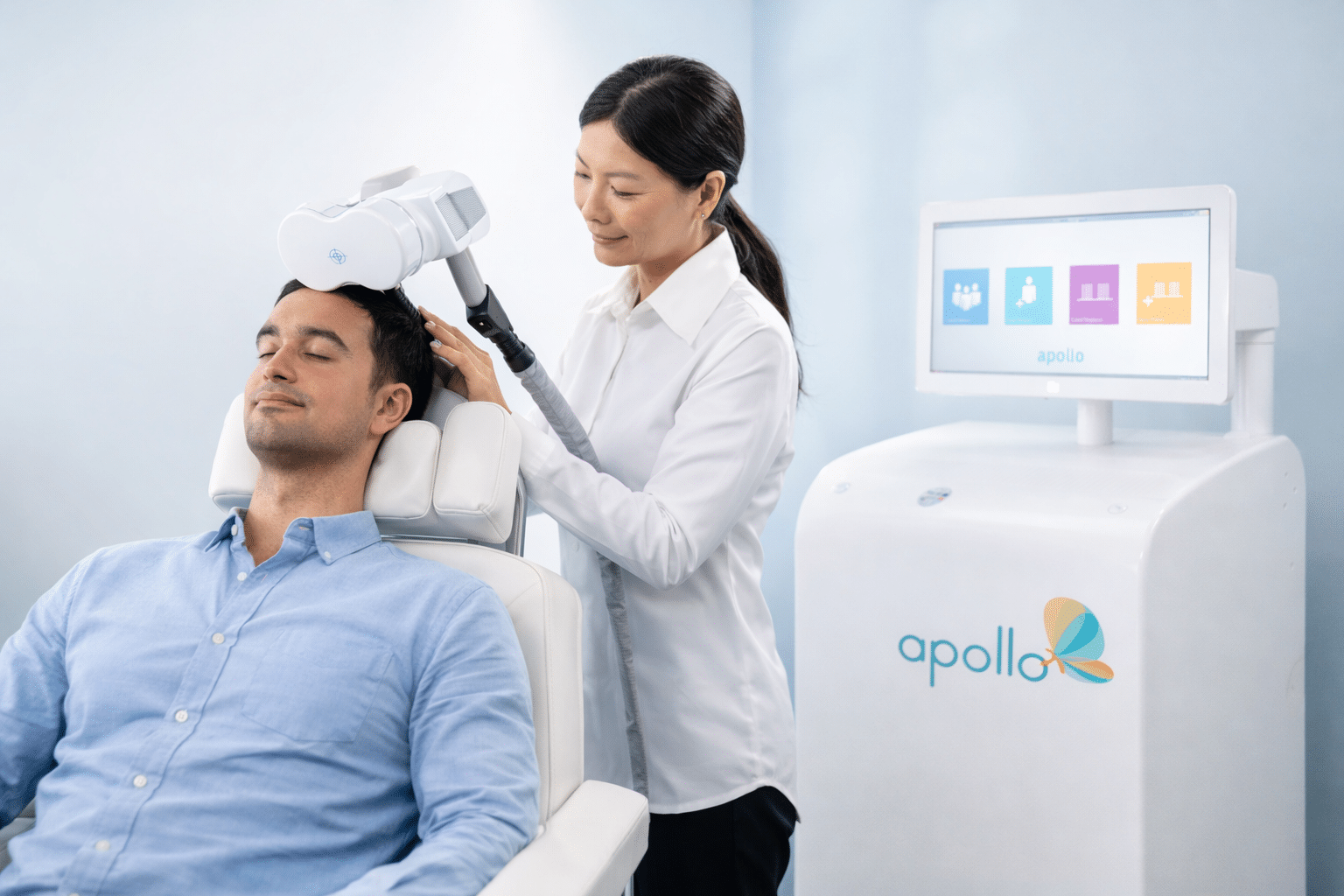
Many individuals who consider transcranial magnetic stimulation (TMS) are already taking medication, have tried medication in the past, and/or are engaged in psychotherapy. In clinical practice, combining medication with TMS therapy is often a thoughtful and intentional approach rather than an indication that treatment has failed.
Mental health conditions such as depression affect multiple aspects of brain function and daily life. Because of this complexity, care frequently involves more than one treatment approach working together to support recovery.
Understanding How TMS and Medication Work Together
Medication and TMS influence mental health through different mechanisms. Medication acts broadly on brain chemistry and can help stabilize mood, reduce symptom intensity, and support emotional regulation. For many individuals, this provides an important foundation for daily functioning.
TMS, in contrast, targets specific brain regions involved in mood regulation. Through focused magnetic stimulation, TMS helps modulate activity in neural circuits that may be underactive in depression. Rather than affecting the entire body, it works directly on patterns of brain activity linked to mood and motivation.
This combined approach has been examined in research. A recent study and meta-analysis of randomized controlled trials found that individuals who began active TMS alongside antidepressant medication experienced greater short-term improvement in depressive symptoms compared with those receiving medication with sham stimulation. These findings support combining medication with TMS therapy as a considered clinical strategy rather than a last-line option.
Why Combining Medication With TMS Therapy Can Make Sense
In some cases, medication alone may reduce symptoms without fully restoring motivation, concentration, or emotional flexibility. Others may experience partial response or diminishing benefit over time. In such situations, adding TMS can provide additional support through a different therapeutic pathway.
Clinical experience and research suggest that combining medication with TMS therapy may be considered when depression affects multiple aspects of daily functioning, such as:
- Persistent low mood despite medication use
- Difficulty with motivation, focus, or emotional responsiveness
- Partial improvement that plateaus over time
Additional evidence highlights the importance of personalization. A systematic review examining antidepressant classes used during TMS found higher response and remission rates among individuals receiving TMS alongside SSRI medications compared with medication plus sham stimulation. The authors noted that outcomes were not uniform across all medication types, reinforcing the need for individualized treatment planning
Taken together, this evidence helps explain why combination care is often considered. The goal is not to intensify treatment unnecessarily, but to align care with how symptoms affect functioning and quality of life.
Where Therapy Fits Into a Holistic Treatment Plan
While medication and TMS address biological aspects of depression, psychotherapy focuses on emotional patterns, behavior, and coping strategies. Therapy provides space to process experiences, develop insight, and build skills that support long-term stability.
For some individuals, combining medication with TMS therapy may make psychotherapy more accessible and effective. As symptoms such as fatigue, hopelessness, or impaired concentration improve, engagement in therapeutic work may become more productive. A holistic treatment plan recognizes that recovery involves both brain-based and experiential change.
What Patients Often Worry About When Combining Treatments
When more than one treatment is recommended, it is common for individuals to have concerns or questions. These worries often include:
- Whether combining treatments means their condition is severe
- Concern that previous treatments were unsuccessful
- Uncertainty about the need for ongoing or long-term care
In clinical settings, these concerns are addressed through collaborative discussion and ongoing evaluation. Combining treatments typically reflects individualized decision-making rather than escalation. Mental health recovery is rarely linear, and adjustments to care are a normal and responsible part of treatment.
What a Personalized Treatment Roadmap Looks Like

There is no single roadmap that applies to every individual. Some continue medication during TMS, while others make adjustments later under clinical guidance. Psychotherapy may remain consistent or shift focus as symptoms and goals evolve.
What remains consistent is collaboration. Treatment decisions are revisited over time, progress is monitored, and care is adapted based on response and tolerability. This flexible approach supports both short-term symptom relief and longer-term well-being.
Final Thoughts
Mental health recovery is rarely about selecting one treatment in isolation. For many individuals, progress involves combining approaches that support brain function, emotional health, and daily life together. Combining medication with TMS therapy reflects a holistic and patient-centered approach to care.
This approach does not indicate failure. More often, it reflects care that is being thoughtfully tailored to an individual’s needs, history, and response to treatment. With guidance from a licensed mental health professional, it is possible to move forward with a plan that supports meaningful and sustainable improvement.
Frequently Asked Questions (FAQs)
1. Can medication be continued during TMS treatment?
In many cases, individuals continue their prescribed medication while undergoing TMS, though decisions are made on a case-by-case basis in collaboration with a licensed clinician.
2. Does combining medication with TMS mean depression is more severe?
Not necessarily. Combining treatments often reflects individualized care aimed at addressing symptoms that affect multiple aspects of daily functioning.
3. Can TMS reduce the need for medication over time?
Some individuals may adjust medication as symptoms improve, but any changes should be guided carefully by a prescribing provider based on clinical response and overall stability.
4. Is psychotherapy still important when using medication and TMS?
Yes. Psychotherapy remains an important part of care, as it supports emotional insight, coping skills, and long-term resilience alongside biological treatments.
Responsibly edited by AI
Other Blog Posts in
Animo Sano Psychiatry is now serving patients across multiple states. If you’d like to schedule an appointment, please contact us to get started.
Get Access to Behavioral Health Care
Let’s take your first step towards. Press the button to get started. We’ll be back to you as soon as possible.ecovery, together.